Fungi are nearly everywhere in nature and play a crucial role in breaking down organic matter into smaller components.
Their attraction to dead plants allows nutrients to be released into the soil when the plants decompose.
Generally, fungi don’t infect animals because of the warm body temperature and dryness.
Read Also

Here’s a dairy lactation feed budget to consider for 2026
By using current prices for forages and other feeds and implementing some cost-cutting measures, I can draw a picture as to what it actually costs to feed a lactating dairy cow.
However, specific fungi, known as dermatophytes (derm-at-o-fights), infect the outer layers of the skin and hair, leading to a disease known as ringworm. It is important to note that there are no worms involved in ringworm.
From a biological perspective, this makes sense because hair and outer skin are essentially dead tissue.
As skin cells mature, they lose their genetic material and transform into a thin layer of keratin, which is the strong protein that makes hoofs and claws hard and forms an important component of the skin’s protective barrier.
Horses, cattle, dogs and cats are commonly affected by these skin fungi. It can also occur in sheep, pigs and even alpacas.
The fungi tend to be highly contagious and will spread among a group.
In cats, they are particularly an issue for shelters and in hoarding situations where animals are stressed, grooming equipment may be shared and animals may be crowded.
The name ringworm comes from how the disease looks and progresses.
Initial lesions are areas of hair loss, often on the face.
Next, the skin may be covered in scale that looks like dandruff and eventually, a thicker white to grey crust.
This can spread to the rest of the skin in severe cases and may or may not be itchy.
The body’s reaction to these fungi corresponds to the changes visible on the skin.
The fungi invade and destroy the part of the hair that is past the bulb and makes the hair extremely fragile and prone to breaking off. This leads to an area of hair loss.
The infection also targets the outer layer of the skin.
As the body’s immune system detects the invaders, it clears the infection in the middle, but the fungus can spread outward, creating an irregular or circular lesion. The immune response stimulates increased blood flow to the lesion, creating an outer red rim.
Fortunately for animals, these fungi do not usually infect the deeper tissues.
While the lesions don’t look particularly nice, they are usually of minimal consequences to the animal and often resolve on their own.
In some cases, fungal damage to the skin allows bacteria to overgrow and invade, which can lead to secondary skin infections that are more serious and challenging to treat.
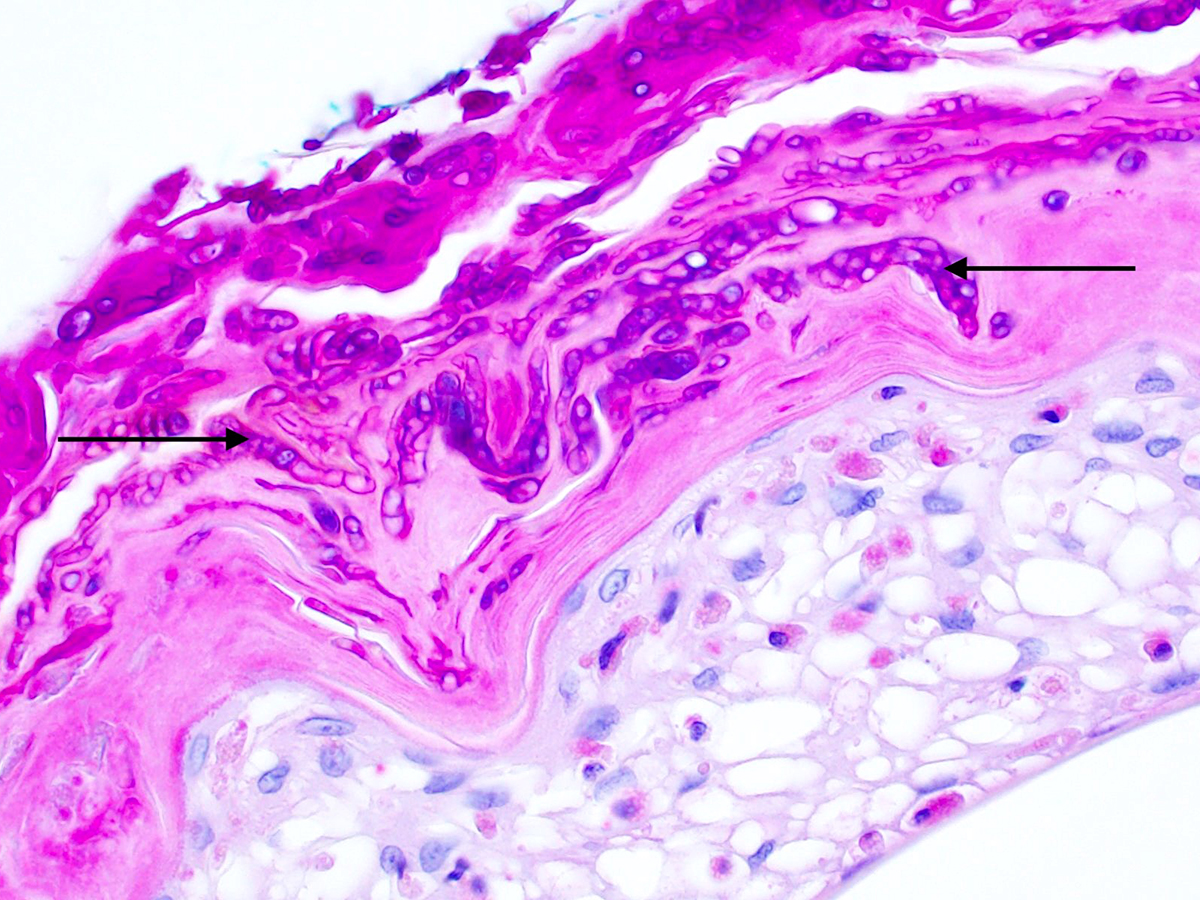
Diagnosis is based on the appearance of typical lesions in combination with viewing hair and scales under the microscope to see the fungi.
Infected hair glows bright green under a special ultraviolet lamp, which can also support the diagnosis.
A skin biopsy and culture can confirm the presence of fungi and the species involved.
Treatment involves clipping the hair to expose the skin and using medication and rinses directly on the skin to kill the fungi.
Dogs and cats can also be shampooed with anti-fungal shampoos and administered oral medication. It can take weeks to months to resolve.
Transmission occurs between animals through contact or via contaminated objects such as halters, brushes and other equipment.
Infection is thought to require some type of predisposing factor such as damage to the skin from clipping, lack of sunlight exposure, moist conditions or severe stress.
Young animals are also at the highest risk of infection.
Fungi that infect the skin of animals are usually zoonotic, meaning people can get this infection from animals.
Contact with infected animals is how it spreads to people, making farmers, family members and veterinarians most at risk.
From a global perspective, there has been a general increase in fungal disease among animals, which may be driven by climate change factors, making the possibility that these domestic animal infections may increase in frequency here as well.